Lung Cancer Is A Major Public Health Problem
Lung cancer is the leading cause of cancer death in the United States, and the leading cause of cancer death among men and women, but it doesn’t have to be. Few preventive interventions are as reliably effective in reducing avoidable death as screening for lung cancer.
235,760
Estimated adults diagnosed with lung cancer in 2021
131,880
Estimated deaths from lung cancer in 2021
1 in 15
Adults ages 55-80 who report getting screened as recommended
Lung Cancer Screening Rates
It takes time to introduce a new screening test, and current self-reported rates of having undergone a low-dose C.T. examination for lung cancer are very low. We are tracking all major measures to assess our progress in uptake of lung cancer screening (LCS) among eligible adults.
A recent study led by the American Cancer Society examined annual LCS rates before (2019) and during (2020) the COVID-19 pandemic nationally and by state.2 The data show that national LCS rates remained stable between 2019 and 2020, and just under 1 in 15 eligible persons were screened. Among 8.51 million eligible adults, only 564,164 and 557,795 adults received LCS in 2019 and 2020, respectively. Data indicate that the lack of nationwide declines could be due to the underutilization of LCS before the pandemic began, when only 5-6% of adults received screening in 2018, limiting the room for further decreases.
Furthermore, states’ stay-at-home orders and COVID-19 surges may have influenced short-term screening volumes, though there was not a clear pattern with annual LCS rates. During the same period, screening rates were unchanged in 25 states.
Although national LCS rates decreased in some states, overall LCS rates remained low and unchanged, and 19 states experienced significant improvements in screening rates despite the COVID-19 pandemic. In five states (Utah, Rhode Island, Vermont, Hawaii, and Maryland), LCS significantly decreased by 23-52%, including some with lower LCS rates before the pandemic.
Screening rates, however, increased between 2019 and 2020 for 19 states, suggesting that health systems and local and state-level cancer control efforts played a role in improving LCS. For example, Kentucky, which has one of the nation’s highest LCS rates, has made concerted efforts to improve LCS since 2013. Lung cancer remains the leading cause of cancer death in the United States, and annual LCS with low dose computed tomography (LDCT) is recommended for a group that is at a high risk of dying from this disease
CDC’s Behavioral Risk Factor Surveillance System (BRFSS)
In 2017, CDC included an optional module (Module 21) in the BRFSS. Respondents will be asked about smoking history, whether they had a CT scan in the previous 12 months, and whether the scan was to check for lung cancer. States that included Module 21 will have state-wide estimates of recent lung cancer screening.
National Health Interview Survey (NHIS)
The NHIS is a nationwide survey that produces national estimates of health indicators. The NHIS includes a cancer control supplement (CCS) every 5 years, and the most recent CCS was conducted in 2015. In 2010, only 3.3% of adults who met USPSTF criteria for lung cancer screening reported having undergone lung cancer screening; in 2015, only 3.9% reported having undergone lung cancer screening.2 The next CCS is scheduled for 2020.
State and Local Level Statistics
The following sources provide comprehensive cancer data by state, county, and city levels for the major cancers. Data specific to lung cancer are highlighted:
- Cancer Facts & Figures, 2021 (ACS) – national- and state-level lung cancer incidence and mortality rates, projected number of new cases and deaths, risk factors, including the most current data on tobacco use, an update on clinical trials, and the U.S. Preventive Services Task Force lung cancer screening recommendation, appropriate treatment, and survival rate.
- Cancer Prevention & Early Detection Facts & Figures 2021-2022 (ACS) – national- and state-level statistics on adult and youth tobacco use, including smokeless tobacco and E-cigarettes, national trends in tobacco use, cessation statistics, comprehensive tobacco control measures by state, and other statistics. A short section on lung cancer screening also is included.
- Cancer Statistics Center (ACS) – state-level incidence and mortality rates
- State Cancer Profiles (NCI) – county-level incidence and mortality rates
- United States Cancer Statistics: Data Visualizations (CDC)state and national incidence and mortality data and maps
- Trends and Patterns of Disparities in Cancer Mortality Among U.S. Counties, 1980-2014 – county-level mortality data and maps
- 500 Cities Project (CDC) – current smoking rate estimates for 500 major U.S. cities; city by city comparisons can be made
- Lung Cancer Screening Locator Tool (ACR) – locations of American College of Radiology lung cancer screening center locations and ACR Designated Lung Cancer Screening Centers that exceed basic equipment, personnel, and imaging performance requirements for providing lung cancer screening services.
Lung Cancer Incidence & Mortality
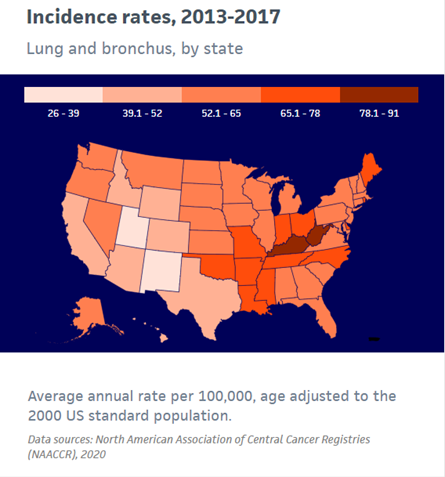
Lung cancer incidence has been declining since the mid-1980s in men, but only since the mid-2000s in women because of gender differences in historical patterns of smoking uptake and cessation. Since the mid-2000s, the incidence has decreased steadily by about 2% per year overall, but at a faster pace in men than in women.
Mortality trends: Lung cancer mortality has declined by 54% since 1990 in men and by 30% since 2002 in women due to reductions in smoking, with the pace accelerating in recent years; from 2014 to 2018, the rate decreased by more than 5% per year in men and 4% per year in women.
U.S. Lung cancer incidence rates, 2013-2017
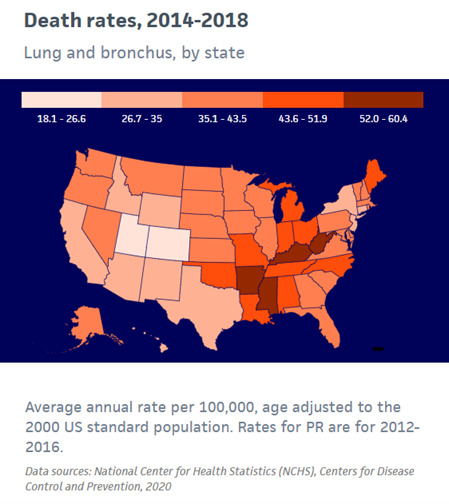
U.S. Lung Cancer Mortality Rates, 2014-2018
State and Local Level Incidence & Mortality Rates
The following sources provide state, county, and city level incidence and mortality rates:
- Cancer Statistics Center (ACS) – state-level screening, incidence, and mortality rates
- United States Cancer Statistics: Data Visualizations (CDC) – state and national incidence and mortality data and maps
- Surveillance, Epidemiology, and End Results (SEER) (NCI) – The SEER Program provides information on U.S. cancer statistics to reduce the cancer burden among the U.S. population. The SEER site provides reports on cancer, interactive tools, maps, and graphs, and tutorials on cancer statistics. Data is updated yearly.
- State Cancer Profiles (NCI) – county-level screening, incidence, and mortality rates
- Trends and Patterns of Disparities in Cancer Mortality Among U.S. Counties, 1980-2014 – county-level mortality data and maps
Sources
- Cancer Facts & Figures 2021. American Cancer Society, Atlanta, GA.
- Fedewa SA, Bandi P, Smith RA, Silvestri GA, Jemal A. Lung Cancer Screening Rates During the COVID-19 Pandemic. CHEST. doi: 10.1016/j.chest.2021.07.030.